“No sugar, but quite milky for me, please.”
“I don’t make many cups of tea,” says Richard, searching for tea bags at the back of his kitchen cupboard. “I can’t normally cope with the organisation of it. I’m only managing now because you’re prompting me.”
I remember now. When I sat with Richard at his Work Capability Assessment some months ago he mentioned that his ADHD affected even the smallest of tasks. His addiction to cannabis and alcohol wouldn’t have helped either.
Richard lives alone in one of a couple of dozen housing association flats that surround a converted nursing home set in large, pleasant gardens. “How long have you lived here?” I ask.
“I moved from Preston about a year ago, to get away from the madness,” he says, “forgetting that the madness was actually me.”
“I like that line,” I say. “I’ll use that.” We both laugh.

Richard went into detox a few weeks after the ATOS assessment – to come off the alcohol and cannabis – but has since had notification that, in the opinion of his assessors, he is fit for work.
“They basically said that because I volunteer for two hours a week at the UCAN then I should be able to work. It feels as if I am being punished for my honesty in telling them about the volunteering. I don’t want to lie to them.”
“I’m no expert,” I say, “but I think what you need right now is some support, never mind the hassle of appealing against the decision. You’re going in the right direction and, in a year or so, you’d be much better placed to look for work.”
We’re in his sitting room now, the TV on mute. “So how was detox?” I ask.
“It was a struggle,” he says, “there was a lot of shaking, retching and sweating for three weeks but I got through it.”
“And now you’re effectively doing your rehab back in your own flat?”
Richard nods as he lights his roll-up. “I have to say that after 20 years of constantly using, I do miss it.”
“That’s to be expected isn’t it?”
“I suppose so. But it’s like the cannabis and alcohol have a voice and are constantly trying to draw me back. It’s hard to shut my head up. I have to put music on or go for a walk just to distract it. Sometimes It refuses to be distracted. It can be quite frustrating.”
“And what support are you getting?”
Richard says he goes to a couple of groups with his local drug and alcohol team as well as with Alcoholics Anonymous. “And everyone at the UCAN is very supportive,” he says, genuinely. “But it’s hard, very hard. It had such a hold over me. It controlled me, literally. It controlled what time I ate, what time I went to the toilet, what time I went to bed, if I could go to bed. And now there’s a massive void.”
“Yes, but think of all the things you can do to fill that void,” I suggest.
“Which I am doing, quite successfully.” Richard, who loves the outdoors, has joined a walking club. “Maybe I should give myself a pat on the back for that.”
There’s a large carrier bag from the chemists on the sofa next to him.
“Is that your medication?” I ask.
Richard pulls out a number of jumbo-sized blister packs, each compartment filled with tablets and capsules of different colours and shapes. “Does the pharmacist organise all these for you?”
“Yeah, because of my ADHD.”
“And what are you on?” Richard reels off a list of seven or eight medications and the conditions which they treat.
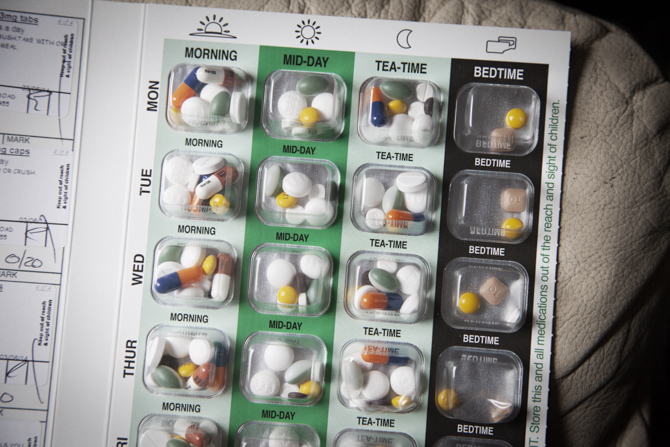
“I have to take one… two… three… ” he counts the contents of several doses, “twenty-four… twenty-five… about thirty tablets a day. As well as Disulfiram, the anti-booze drug which makes you very ill if you intake any alcohol.”
“And have you taken this morning’s tablets?”
“No, actually I need to take them… right now.” He gets a glass of water from the kitchen.
“It’s a good job I’m here,” I say as he fills the palm of one hand with tablets.
“Yes, it is a good job you are here, actually.”
…continued from Fit for work?
At the hospital we eventually find the right place and are promptly ushered into a standard consulting room where a pleasant nurse – she tells us later she used to work on a drug and alcohol team – explains the procedure and starts asking questions.

She works through each of Richard’s symptoms: ADHD, alcohol dependency, hearing loss, anxiety and depression, and asthma and asks the same questions for each, typing his responses. “What are the symptoms of your ADHD?”
Richard is nervous. “Lack of concentration, confusion,” I recall he says.
She asks who diagnosed the condition, when, what tests did they do? When was the last time he saw a medical professional about this condition? She asks about his medication and then a series of standard questions about his daily routine. Can he cook for himself? Can he use a microwave? Can he wash himself? How often does he use the toilet at night?
The questions are rigid and formulaic. When she asks if he can use a microwave to heat and cook food Richard replies he can’t cook but he does heat food. “I can’t differentiate,” she says, “I’ll put down, cook and heat.”
The inadequacies of these ATOS assessments are well documented elsewhere but the irony of Richard’s situation isn’t lost on me. His ‘headline’ symptoms are an inability to concentrate and a tendency to get confused and here he is, sitting on the edge of his chair, being expected to articulate expansive answers to these quick fire questions and build his own case for staying on a disability benefit.
Throughout the half hour assessment the nurse makes it clear that she is not the one who will make the final decision. That will be left to a Department of Work and Pensions case manager who will read the report having never met Richard.
“I was expecting to be able to go into more detail about my own personal circumstances,” he says on our way back. “There should have been more on the emotional side, how ADHD affects me.”
“Although I barely know you Richard, I think I found out more about you in our thirty-minute journey there than she did in that formal interview.”
“You’re right. You did. I was much more relaxed.”
“Do you think you can work?” I ask.
“My concentration levels only allow me to do things in small quantities. It would need to be something I enjoy, something I can focus on. Anything boring or mundane, then I just wouldn’t be able to stick with it.”
“And as it stands now, you’re an alcoholic. Do you think you could actually hold a job down? Could you leave the house at eight and come back at six without having a drink?”
“No. No, I couldn’t.”
His appointment is at 9am at the Royal Blackburn Hospital, two buses and a train away or half and hour in the car.
Richard can’t manage public transport on his own. He gets panicky. He’d asked his social worker and his alcohol team worker. Both were unavailable to take him which is where I stepped in. He gets a much-needed lift, I get another story for this blog.
So now, having met in a Morrison’s car park, we’re driving through the East Lancashire countryside in the rain, discussing his ADHD (Attention Deficit Hyperactivity Disorder).
“How does it affect you on a daily basis?” I ask.
“My concentration levels are really, really low,” he says. “I’m always thinking of 100 things at once and I can’t stop it. It’s very frustrating. I can’t organise myself.”
“So what are you thinking about now, as we’re talking?”
“I’m thinking about this wonderful scenery, about the detox and about the questions they are likely to ask me this morning.”
Because of his ADHD, his alcohol dependency and his depression and anxiety, Richard currently receives Employment Support Allowance, a benefit which means he’s unfit for work. However, he does volunteer at the UCAN on a Monday afternoon, helping IT freelancer, Charlotte get people online.
As part of the welfare reforms, he has a controversial ATOS interview this morning to assess whether he should be put on a different benefit.
In 300 yards turn left.
“I’ll give you another example,” he says. “I can completely zone out. I might start crossing a road and not realise it. It’s a miracle I haven’t been knocked over by now.”
Richard is 34 and he tells me he’s been drinking and using drugs since he was 14. “The last 10 years have been full-on addiction but I’ve only admitted it these past five years.”
He’s waiting to be admitted on a three-week hospital detox, although it’s not the first time he’s tried to stop.
“I’ve come off in the past, just to prove a point, but that’s not the same, is it? This one is for me. Because I want to change.”
As well as the detox, his psychiatrist has changed his ADHD medication and booked him on Cognitive Behavioural Therapy sessions – talking therapy – for the next couple of years.
“You’ve got quite a journey ahead of you, haven’t you?”
After 300 yards turn right and then bear right.
“I’m scared though. Because alcohol is all I know. It’s going to be hard.”
Richard’s two-hour volunteering session at the UCAN is a lifeline at the moment, the highlight of his week. “I went to do an IT course there and was shocked when Charlotte asked me to volunteer. I can manage it for a couple of hours and, because it’s something I’m passionate about, I can focus on it for that short time. Now I’m buzzing.”
In 300 yards, you have reached your destination.
Continued in “Do you think you can work?”
Morag is easy to talk to. She must have told her horrific story to plenty of professionals over the last 27 years, so re-telling it to me over a hot chocolate in Morrisons is not an ordeal. She admits, though, she hasn’t got ‘closure’ on much of it and gets upset recalling particular details.
Morag tells me about the violence back home in Glasgow, the calls to the police, the terrifying ordeals, one after another. “He had a knife to my throat,” she says, reaching for another tissue. “As soon as I could, I fled but my baby was still inside, with him. It was four days before the police could get in and I got my daughter back.”
Her husband ended up in prison but not, ironically, for the violence he heaped on her. There’s more to this story than is necessary to tell.
“For six months, I wouldn’t leave the house. I tried but I couldn’t move. One day I walked to the local shop but it felt like the walls were moving in on me.”
“My cousin was in Bolton and suggested I moved down here, for a fresh start, so I did. My daughter still hadn’t started school and I couldn’t afford childcare so I went to college. There was no way I was sitting around doing nothing.”
But despite her best efforts Morag couldn’t get back on her feet. She was hospitalised after her stomach muscles fused together. “He never touched my face,” she recalls, “instead he’d kick me in the stomach. Always the stomach. I had to have emergency surgery.”
She was diagnosed with post traumatic stress disorder and spent more than a decade on medication.
“I thought everything was okay, but I was just plodding along, getting my daughter to school. But she was really the one looking after me. Every morning she’d ask me if I’d taken my tablets.”
“How old was she at this point?” I ask.
“Five,” says Morag.
“So, let me get this right. That violent relationship has affected you, both mentally and physically, for the past 27 years?”
She nods. “And last year I got a call to say that my money was stopping and I had to apply for another benefit.”
Morag is one of tens of thousands of disability benefit claimants who have been assessed under the government’s work capability assessment programme in a drive to get people into work and reduce welfare payments.
She was questioned by Atos Healthcare, the private company commissioned by the Department of Work and Pensions, and was subsequently declared fit for work. She appealed against their decision and attended a tribunal.
“It was terrifying,” she says. “There was a Justice of the Peace and a medical examiner and they fired questions at me for an hour. At the end of it they said they were going to fail my appeal. And that was it. I was on Jobseeker’s Allowance and had £160 less each month.”
“Do you feel you are fit for work?”
“I do and I don’t. I want to work. I’m sick of relying on benefits.”
“And now you’re on Jobseeker’s Allowance and living off £15 a week after you’ve paid your bills?”
“But I’ve got absolutely brilliant friends. They give me bits of food and clothes. They gave me this,” she says, tugging at her coat. “But I don’t know how anyone would cope if they didn’t have the friends I had. How would they manage?”
“And how helpful has the UCAN Centre been?”
“I just love them. They’ve really helped to build up my confidence. I’m not there yet but I’m nearly there… we’re nearly there. The course I did with Cath was brilliant. I didn’t know myself. It’s opened my eyes.”
It turns out that, as well as the employment support, Morag is about to tap into the counseling service that comes to the UCAN every week.



